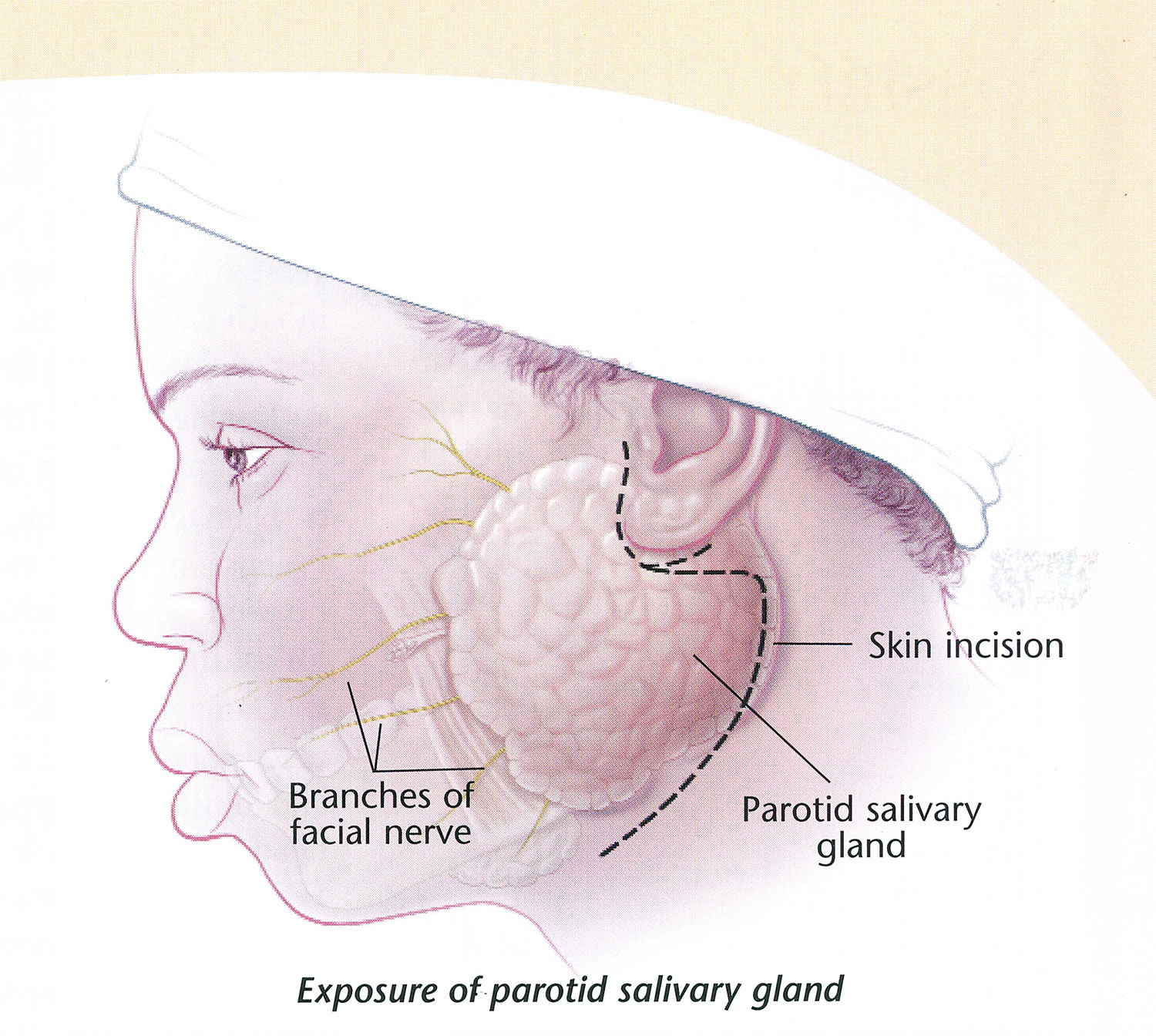
The facial nerve and parotid gland surgery
The facial nerve runs through the parotid gland like a skewer through an apple. During parotid gland surgery, the surgeon starts by locating the facial nerve behind the gland then follows the nerve carefully through the gland, to allow removal of the gland without damage to the nerve. A nerve monitoring device is used during surgery. This reduces the risk of damage to the nerve but can’t guarantee it won’t be damaged.
The facial nerve makes the muscles on one side of the face move. This includes closing the eye and lips and making facial expressions like smiling and frowning. If the facial nerve is damaged, one half of the face doesn’t move. This can be complete (no movement at all, paralysis) or incomplete (reduced movement). It can affect all the muscles of the face or just some of the muscles.
The most important function of the facial nerve is blinking and closing the eye. This is essential to keep the surface of the eye healthy. If a facial nerve injury happens, protecting the eye is the most important thing to do, to prevent change in vision.
6:100 people have temporary weakness in the muscles on one side of the face. This can last for up to 12 months.
1:100 people have permanent weakness in the muscles on one side of the face. There are procedures that can make the face look more symmetrical and to help the eye close, but procedures can’t make the muscles move normally again.
Other temporary side effects:
The skin around the wound and ear is always numb after surgery. For most people this gradually improves over 6 months.
3:100 people develop a collection of saliva under the skin (sialocoele) 1-2 weeks after surgery. This usually improves with wearing a pressure device. Occasionally it needs to be aspirated with a needle.
1:100 people have bleeding into the wound within 24 hours of surgery. If this happens, you will be taken back to the operating theatre to have the blood vessel sealed again.
Less than 1:100 people have an infection in the wound and need tablet antibiotics
Clots in the legs (deep vein thrombosis) can rarely occur. Prevention starts in hospital with TED stocking, compression devices on the legs and injections of medication.
Other permanent side effects
Sometimes numbness in the skin is permanent
Rarely, the scar is unattractive and needs to be improved with another operation
Less than 1:10 people have Freye’s syndrome (sweating on the side of the face when eating). It is often minor and easy to tolerate. If it is more severe, it can be treated with injections into the area to stop the sweat glands working.